- Personalized care for terminally ill patients improves quality of life through tailoring treatments to individual needs.
- Effective communication between healthcare providers, patients, and families is key to understanding and meeting diverse needs.
- Technological solutions, like shared electronic health records, enhance coordination and ensure personalized, holistic care plans.
- Emotional and psychological support through counseling and support groups is crucial for patients and their families.
- A holistic approach to care honors each patient’s unique life, ensuring dignity and compassion in their final days.
Nurturing the final stages of life is an endeavor that requires empathy, commitment, and a deep understanding of the terminally ill patient’s needs. In a healthcare landscape often shaped by its efficiency and volume, personalized care stands out as a beacon of hope and comfort. But how do we ensure that patients with terminal illnesses not only receive treatment but also experience a life of quality and dignity in their final days? This article unravels the pathways to providing personalized care, a roadmap that balances medical management with emotional and environmental needs.
Understanding Personalized Care for Terminally Ill Patients
The term’ personalized care’ is not a novelty, yet its application in the context of terminal illness is a topic that’s often overlooked. In this instance, personalized care involves tailoring healthcare delivery to meet patients’ needs, preferences, and values. It means moving beyond conventional or standardized treatment to provide a plan that reflects who the person is, what they’ve enjoyed in life, and how they wish to be treated.
The Role of Comfort and Familiarity in Personalized Care

The setting in which a person spends their last days can significantly affect their well-being. For many, being surrounded by the familiar—the comfort of their home, the faces of loved ones, or the belongings that tell their life story—can bring peace and dignity. This environment isn’t always a hospital or hospice room; specialized home service healthcare providers can maintain it at home. They can offer medical care and emotional support and ensure the patient’s home environment remains conducive to their needs.
The Importance of Emotional Support in Personalized Care
Dealing with a terminal diagnosis is not only a physical ordeal; it is an emotional and psychological one as well. Families and loved ones are the primary sources of emotional support, providing comfort, care, and companionship. Professional counselors and support groups can also play a vital role, offering a space to address fears, express feelings, and find ways to cope during this difficult time.
The Value of Customized Medical Attention in Personalized Care
Each patient is unique, and their medical needs are equally distinct. Customized medical attention involves tailoring medications and treatments to the patient and ensuring schedules are designed for the best possible comfort and quality of life. It’s about focusing on the person first and the diagnosis second, a principle that guides the approach to personalized care.
Practical Ways to Implement Personalized Care for Terminally Ill Patients
From the family’s perspective, practical personalized care can start with simple steps. Understanding the patient’s wishes, creating a comfortable living space, and ensuring medical treatments align with their goals can go a long way. Healthcare professionals, on the other hand, must engage in open, honest conversations with patients, listen to their concerns, and provide medical help and genuine support.
The Impact of Personalized Care on End-of-Life Journey
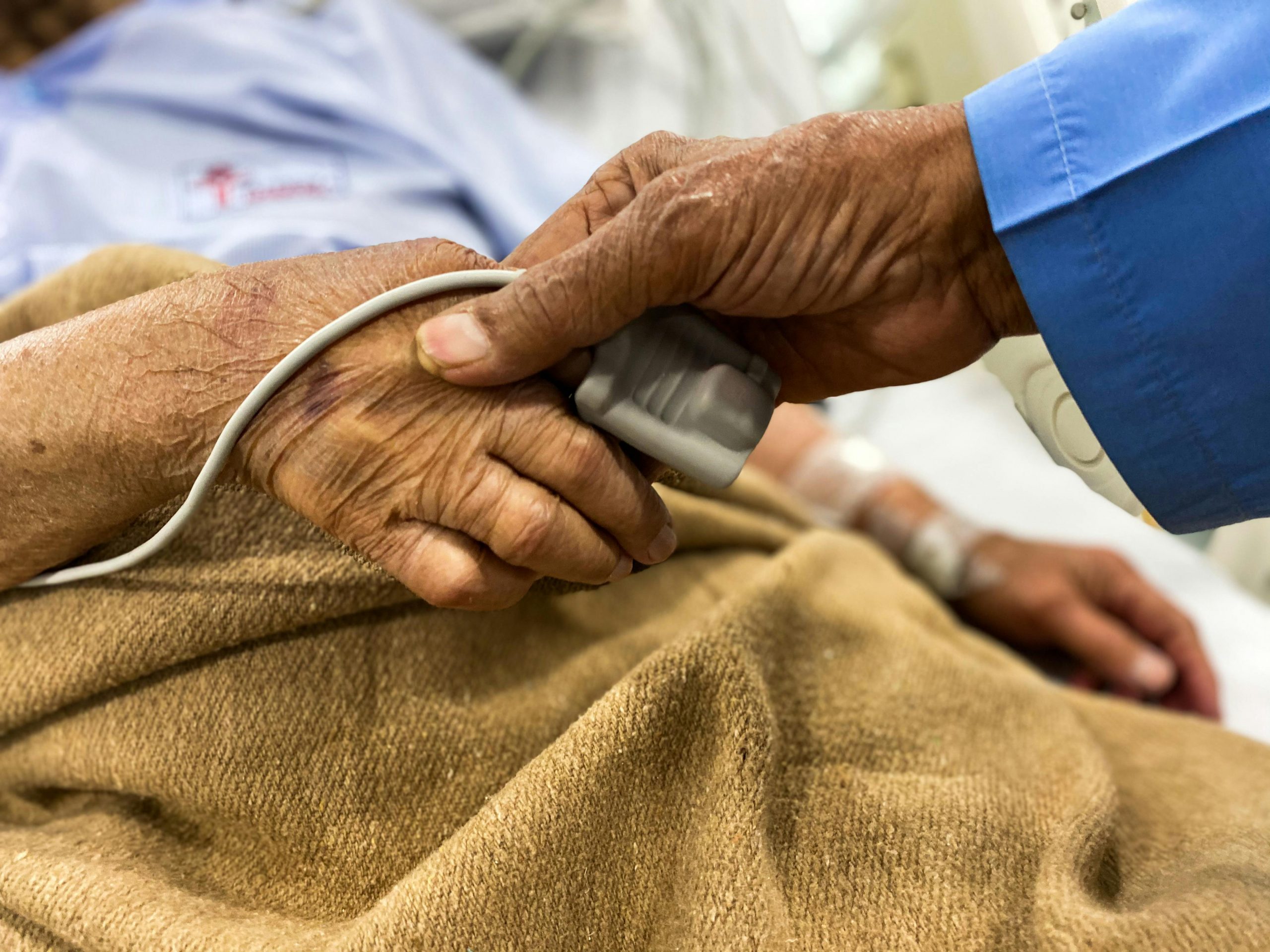
As a patient’s condition deteriorates, the focus shifts to end-of-life care. Patients and their families can experience more meaningful moments by incorporating personalized care throughout their journey. This approach recognizes that every patient’s final days are unique and tailors treatment plans accordingly. It also gives patients a sense of control and dignity during a difficult time, allowing them to address fears, express feelings, and find ways to cope. Ultimately, personalized care helps patients make the most of their remaining time and improves overall quality of life. Overall, personalized care is vital in providing comfort and support to patients and their loved ones during the end-of-life journey.
Challenges and Solutions in Providing Personalized Care
Despite the clear benefits personalized care offers to terminally ill patients, implementing it effectively presents several challenges. However, these can be addressed with thoughtful solutions.
One prominent challenge is the standardized nature of healthcare systems, which often prioritizes efficiency over individualized attention. Healthcare professionals may be constrained by strict schedules and protocols, limiting their ability to spend much-needed time with each patient. To circumvent this, healthcare facilities can adopt more flexible scheduling systems and increase staffing levels, affording caregivers more time to engage with patients personally.
Another significant issue is healthcare workers’ lack of training in personalized care approaches. While medical professionals are exceptionally skilled in clinical treatments, they might not always be equipped with the necessary skills to offer the emotional support terminally ill patients need. Implementing comprehensive training programs that include communication skills, empathy development, and patient-centered care techniques can make a considerable difference in this area.
Furthermore, integrating personalized care into the healthcare system requires effective collaboration among a multidisciplinary team. Ensuring seamless communication and understanding among doctors, nurses, counselors, and social workers can be challenging but is crucial for providing comprehensive care. Employing technological solutions like shared electronic health records and regular interdisciplinary meetings can enhance coordination and ensure that patient care plans are truly personalized and holistic.
Lastly, addressing patients’ and their families’ emotional and psychological needs is a complex facet of personalized care. It involves acknowledging and managing not only the physical symptoms but also the fears, hopes, and emotional struggles that come with terminal illnesses. Creating support groups and counseling and ensuring that spiritual care services are available can significantly meet these needs.
Each patient’s story must continue with compassion and dignity in the twilight of life. Personalized care for terminally ill patients is not a monolith; it’s a nuanced, collective effort that embraces the uniqueness of each individual’s life. By weaving emotional and environmental elements into the fabric of medical care, you can ensure that the patient’s final chapter is written with the cadence of their life’s story.

